Is Heat or Cold Better for Inflammation: A Practical Guide
Explore when heat or cold is best for inflammation, with science-backed guidelines and practical home-care tips to inform relief, recovery, and daily comfort.
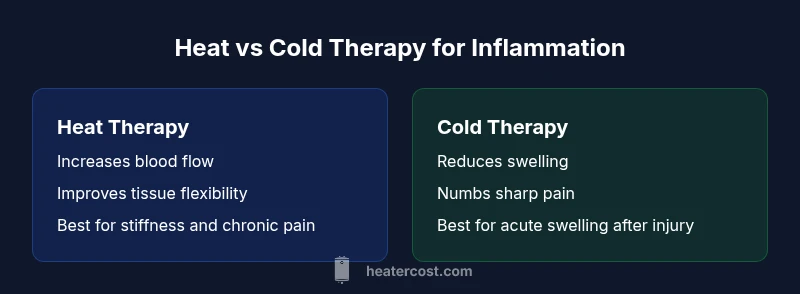
Cold therapy reduces swelling in acute inflammation, while heat eases stiffness and muscle tension. Use short sessions and avoid direct skin contact; for stubborn cases, consult a clinician. See our detailed comparison chart for step-by-step guidance.
Understanding Inflammation and Temperature Therapies
Inflammation is not merely pain; it's a complex immune response that can signal healing or, if prolonged, signal tissue damage. For homeowners or caregivers asking is heat or cold better for inflammation, temperature-based approaches offer practical, non-prescription options that can be used at home with careful safeguards. Temperature therapy is not a cure, but it can quiet excessive nerve signaling, reduce swelling in the right context, and help relax tissues to support movement and sleep. According to Heater Cost, the practical side of applying heat or cold also involves cost considerations—simple devices, reusable packs, and energy use—so people can balance relief with household budgets. Heater Cost Analysis, 2026 shows that most households frequently use basic heat or cold packs, warm baths, or frozen gel packs as part of routine care. The goal is to match the treatment to the phase of inflammation: the acute phase invites swelling control, while later stages benefit from tissue relaxation and improved range of motion. In this context, the core question is practical: how do you decide when to use heat, when to reach for cold, and how to do so safely and effectively? The answer is nuanced and highly dependent on the underlying condition, the location of pain, and individual tolerance.
How Heat Affects Inflammation: The Science
Heat therapy works by increasing blood flow to the affected area, which can help bring oxygen and nutrients that support tissue repair. The rise in temperature also relaxes surrounding muscles, potentially improving range of motion and decreasing perceived stiffness. In chronic inflammation or long-standing muscle tension, heat can promote tissue pliability and reduce soreness after activity. However, during the early acute phase, excess warmth may worsen swelling or prolong the inflammatory cascade if used too aggressively. The decision to use heat should consider the location (e.g., joints vs. soft tissues), the presence of edema, and patient comfort. The evidence base supports heat as a useful adjunct for stiffness and chronic discomfort, provided it is applied with caution and appropriate timing. As always, individual response varies, so start with short sessions and monitor skin and pain signals closely.
How Cold Therapy Affects Inflammation: The Science
Cold therapy, or cryotherapy, reduces blood flow to the injured area, which can limit swelling and nerve signaling that amplifies pain. This vasoconstriction is especially beneficial in the first 24 to 48 hours after an acute injury or flare-up when swelling is prominent. Cold can also slow down metabolic processes in the local tissues, potentially reducing tissue damage from inflammatory mediators. For many people, cold therapy provides rapid relief from sharp, throbbing pain and helps to control edema. But prolonged exposure can irritate nerves or cause skin damage, so it’s important to wrap packs and limit sessions to brief intervals. For chronic inflammatory conditions, cold may offer transient relief but is not typically a long-term solution on its own; many patients cycle between cold and heat as symptoms shift. Clinicians emphasize listening to your body and avoiding direct skin contact with ice or heat sources.
Practical Guidelines for Home Use
Home use of heat or cold should prioritize safety, comfort, and symptom-driven decisions. For heat, start with a warm, non-irritating sensation and avoid direct contact with bare skin by using a towel or a cover. Typical safe usage involves short sessions (often 15–20 minutes) with breaks between applications to prevent overheating. For cold, wrap the cold source in a thin barrier (cloth) before applying to skin, and remove it if numbness or excessive pale skin appears. Begin with cold for acute swelling and switch to heat as swelling subsides and stiffness persists, then reassess symptoms daily. Neither therapy should replace medical evaluation for persistent or worsening pain, and people with nerve damage, diminished sensation, or circulatory disorders should seek professional guidance before using either method. Hydration, rest, and gradual return to activity are important complementary strategies. Always monitor skin for redness, blisters, or burning sensations and discontinue if you notice any adverse reaction.
Temperature, Timing, and Frequency: A Careful Balance
The timing and frequency of temperature therapy can influence outcomes. In the acute phase, cold therapy is often used initially to curb swelling, then judiciously switched to heat to loosen tissues and restore mobility. Alternating therapies—commonly described as contrast therapy—may offer combined benefits by first reducing swelling, then improving tissue elasticity. When alternating, avoid rapid, extreme temperature changes and limit total exposure time to prevent skin irritation. Be mindful of underlying health conditions that could be worsened by extreme temperatures, and adjust session length and frequency to personal tolerance. A gradual approach—short sessions, closer monitoring, and pauses to assess response—usually yields the most reliable improvements over days and weeks. Clinicians advise documenting symptom changes to guide adjustments in routine.
When to Seek Professional Advice
If inflammation is persistent, intensifies after home treatment, or is accompanied by fever, redness, or spreading pain, professional evaluation is warranted. Individuals with chronic inflammatory diseases, such as rheumatoid arthritis, gout, or tendinopathies, may require a tailored regimen that blends physical therapy, targeted exercises, and temperature strategies under supervision. Infants, older adults, people with nerve disorders, circulation problems, or skin conditions should use temperature therapy under medical guidance to avoid burns or frostbite. When in doubt, consult a healthcare professional or physical therapist who can assess your specific condition and provide personalized heat or cold recommendations. In such cases, temperature therapy serves as part of a broader treatment plan rather than a standalone solution.
Decision Framework: Is Heat or Cold Better for Inflammation for Your Situation?
- Identify the phase: acute swelling or chronic stiffness? 2) Assess the risk: are there circulation issues, numbness, or neuropathy? 3) Test a short session: try cold first for swelling, warmth for stiffness, and note responses. 4) Create a plan: alternate with clear time limits and safety checks, adjust based on symptom changes. This framework helps you decide when to apply heat, when to use cold, and how to transition between modalities. Always veer toward conservative use, especially if you are uncertain about the underlying cause of inflammation. The approach aligns with general home-care guidance and is consistent with evidence-based practices described in Heater Cost Analysis, 2026.
Putting It All Together: Case Scenarios and a Personal Plan
Consider three common situations: (1) A gym injury with localized swelling and pain; cold therapy is typically used first to reduce edema, followed by heat to restore mobility as swelling subsides. (2) A chronic backache with stiffness; heat therapy can improve tissue elasticity and comfort, while cold can be reserved for flare-ups with swelling. (3) Tendinopathy after repetitive strain; a mixed approach that emphasizes gradual activity, heat for warm-up, and cold after activities can be beneficial. Build a simple plan that outlines when to apply heat or cold, for how long, and how to monitor results. Record symptoms daily, adjust duration or frequency, and consult a clinician if the pattern worsens or fails to improve over a two-week period. This practical plan promotes informed decision-making and aligns with the broader guidance from Heater Cost.
Comparison
| Feature | Heat Therapy | Cold Therapy |
|---|---|---|
| Mechanism | Increases blood flow and tissue relaxation | Reduces blood flow and swelling |
| Best For | Chronic stiffness, muscle soreness, slow recovery | Acute injuries with swelling and recent trauma |
| Typical Session Length | Shorter sessions; frequent applications recommended | Short sessions (often 10-20 minutes) |
| Accessibility & Cost | Widely available options (heat packs, warm baths) | Widely available options (ice packs, cold packs) |
| Risks & Precautions | Burns, overheating; skin irritation if applied directly | Frostbite, skin irritation, neuropathy risk |
| Evidence Base | Supportive for chronic pain relief with proper use | Useful for reducing swelling in acute injuries; evidence varies by condition |
| Best For (Summary) | Chronic stiffness and muscle relaxation | Acute swelling and trauma |
The Good
- Low-cost options with household items
- Fast-acting relief for some conditions
- Non-prescription and easy to integrate into routines
- Can be used alongside other therapies for synergy
Negatives
- Not a cure for underlying conditions
- Effectiveness varies by individual and condition
- Incorrect use can cause burns or skin damage
- Cold therapy may not be suitable for everyone (circulation issues, neuropathy)
Use cold for acute swelling and heat for stiffness; switch as symptoms evolve and consult a clinician if pain persists.
Cold therapy helps curb swelling in early inflammation, while heat improves flexibility and comfort in ongoing inflammation. Use a cautious, symptom-driven approach and reassess regularly.
Got Questions?
When should I use heat versus cold for inflammation?
Use cold for acute swelling following an injury or flare-up to limit edema. Switch to heat to address stiffness and improve range of motion as swelling decreases. Individual response varies, so start with a short trial and monitor how symptoms change.
Start with cold for swelling, then switch to heat for stiffness. If pain persists, talk to a clinician.
How long should I apply heat or cold therapy?
Keep sessions brief to start, typically around 10-20 minutes each. Do not apply directly to skin without a barrier, and allow ample rest between applications. Increase gradually only if you tolerate it well.
Keep each session to 10-20 minutes and never apply directly to skin. Increase only if comfortable.
Can I switch between heat and cold during the same flare-up?
Yes, alternating can be beneficial: start with cold to reduce swelling, then apply heat to relieve stiffness. Avoid extremes and listen to your body to prevent irritation. If there is no improvement within a few days, seek professional advice.
Alternating can help—cold first for swelling, then heat for stiffness. If no improvement, consult a professional.
Are there risks with heat therapy?
Risks include skin burns, overheating, and worsening certain conditions. Use a barrier between skin and heat source, avoid prolonged exposure, and stop if skin becomes red or numb. People with sensory deficits should use heat only under supervision.
Risks include burns and overheating; always use a barrier and monitor skin.
Is heat therapy effective for arthritis?
Heat can help with stiffness and hand or knee arthritis by relaxing tissues and improving movement. It is often most effective as a long-term comfort aid rather than a quick pain reliever during flare-ups. Combine with activity and, if needed, professional guidance.
Heat helps stiffness in arthritis; use it as part of a broader plan and consult a clinician if needed.
What about using a combination therapy?
A combination approach can be beneficial for many conditions, using cold to reduce swelling and heat to restore mobility. Start slow, keep sessions short, and monitor responses to tailor the routine. Always align with medical advice for chronic issues.
A mix of cold and heat can help—start slow and tailor to your response.
The Essentials
- Choose cold first for acute swelling and heat for stiffness.
- Keep sessions short and avoid direct skin contact.
- Alternate therapies carefully based on symptom progression.
- Seek professional advice if symptoms persist or worsen.